Over the past two decades, the number of radiological examinations and the use of radiation for medical purposes have rapidly increased [1]. This has resulted in increased radiation exposure for medical staff [2]. One of the departments where staff are most exposed to ionising radiation is interventional radiology [2, 3]. This is because fluoroscopy and computed tomography (CT)-guided interventions involve direct contact with the patient during the procedure, resulting in higher staff exposure [4].
Prolonged and continuous exposure to ionising radiation can have severe health consequences, including an increased long-term risk of developing cancer, which, according to population-based risk models, rises proportionally with the cumulative dose received [5]. Therefore, it is important to minimise staff exposure as much as possible without affecting the quality or results of the procedure. This can be achieved by increasing the distance from the patient, minimising exposure time, and using shielding [6, 7]. Personal protective equipment (PPE) used for shielding includes goggles, gloves, aprons, vests, skirts, and thyroid shields [6, 8, 9]. Most PPE is made of lead-based materials, with lead embedded in rubber [6, 10].
The level of radiation protection is determined by the millimetre thickness of lead-equivalent and the energy of the photons used [11]. PPE with a lead equivalence of 0.25 mm or greater can attenuate approximately 96% of secondary radiation if kept in good condition [12]. The protective capacity also depends on the condition of the attenuating layer [6], which can be easily damaged if the PPE is not handled properly [7]. Additionally, the polymer matrix in lead-rubber x-ray protective materials gradually degrades due to ionising radiation, mechanical stress, and oxidation. Ionising radiation breaks chemical bonds in the polymer and generates free radicals, which weaken the structure and react with oxygen, accelerating oxidative embrittlement. Heat and mechanical stress further accelerate these reactions by increasing molecular mobility, contributing to stiffness, micro-crack formation, and general material fatigue. As the matrix deteriorates, the distribution of lead particles may become uneven, leading to localised thinning or delamination and ultimately reducing the protective effectiveness of the material [13]. Once the protective layer is compromised, it does not provide an adequate level of protection, resulting in increased radiation exposure and a higher risk of radiation-induced health complications. However, this increase in radiation exposure may not be reflected in the dosimetry report, as the TLD may not measure it accurately unless the defect is located directly above it [7].
In recent years, several studies have investigated the integrity of PPE used in clinical settings. A study by Kellens et al [6] which assessed the integrity of PPE over four years, revealed that 50% of the equipment had some form of defect. Similar results were reported by Omojola and Xaviera [12] who observed defects in 70% of PPE during a prospective two-week study in 2018. All studies highlighted the need for quality assessment of PPE. Furthermore, several organisations have published guidelines recommending regular quality control. The most commonly proposed technique is radiographic evaluation using either conventional x-ray or fluoroscopy, which is reported to be the most effective but is often time-consuming and associated with increased occupational exposure if a person is present in the room during testing. Alternatively, CT is significantly more expensive but faster and less demanding in terms of radiation protection. Despite these limitations, periodic testing is recommended as it can significantly contribute to radiation safety [14, 15]. Additionally, several authors, such as Lambert & McKeon [16] and Stam & Pillay [17], have proposed various elimination criteria for determining when lead-based PPE is no longer suitable for use in clinical settings. The Lambert and McKeon [16] model proposes using the area of the defect as an exclusion criterion based on dosimetric and financial considerations, as well as the life expectancy of the equipment. In contrast, the Stam and Pillay [17] model considers only the dosimetric aspect, using defect length as an exclusion criterion. Although some countries have adopted their own evaluation and rejection criteria within the framework of radiation protection guidelines, no internationally recognised guidelines proposing specific testing methods or rejection criteria have been issued. The exact protocol for quality assessment of PPE is therefore yet to be determined [7, 18]. This study aimed to assess the integrity of the lead-based coats used in the hospital where the study was conducted, determine the most effective method for detecting deficiencies, and evaluate the impact of damage on the radiation dose received by staff.
The methodology used in this study is described in detail in the following sections. A cross-sectional study was conducted in a hospital in Slovenia in 2023. All assessments were conducted by one researcher to avoid the potential differences in the assessment protocol. Ethics committee approval was not obtained, as patients were not included in the study.
2.1. Study designA study assessing the integrity of lead-based coats was conducted. In total, 64 pieces, regardless of their manufacturer, were examined for irregularities. Specifically, 14 one-piece coats and 50 two-piece coats (vest and skirt), all used in a clinical environment in the same general hospital, were included in the study. According to manufacturing date records, all coats were manufactured within the last 15 years: 2022 (14), 2019 (10), 2017 (6), 2016 (19), 2014 (13), and 2010 (2). Each coat was labelled with an identification number from 1 to 64, ensuring traceability of damage and that the same coats were assessed in both parts of the study. For each coat, the manufacturing date and the lead equivalent thickness on the anterior side—0.35 mm for one-piece coats and 0.50 mm for two-piece coats—were recorded.
2.2. PPE integrity assessmentFour assessment methods—visual inspection, palpation, light source inspection, and x-ray assessment—were performed according to the protocol proposed by DIN 6857–2 [15]. All coats were assessed using all methods. Additionally, the time required to perform each method was recorded.
2.2.1. Visual inspection and palpationCoats with visible blood or contrast agent stains were cleaned with warm water according to manufacturer’s instructions. A visual inspection was conducted to examine the coats for visible signs of tears, wrinkling, and displacement of the protective material. Afterwards, the coats underwent a palpatory examination to assess for palpable cracks and tears in the protective layer.
2.2.2. Light source inspectionCoats were hung in the dark room, and each layer of the protective material was carefully examined using a Würth 1000 lm LED light (Würth Group, Germany) to check for light transmission through the protective layer.
2.2.3. X-ray inspectionX-ray inspection was conducted using three modalities: CT, fluoroscopy, and conventional x-ray. CT assessment was performed with a Siemens Somatom Drive CT unit (Siemens, Germany). After the coats were placed on the examination table, scout images were acquired (120 kV, 35 mAs). Fluoroscopic examination was performed to identify any white spots in the protective layer that would indicate damage. If damage was observed, conventional x-ray imaging was performed with a GE definium tempo PRO x-ray unit (general electric, USA) at 60 kV and 6.3 mAs, acquiring 6–8 images for one-piece coats or 24 images for two-piece coats.
If damage was discovered, its position on the coat was recorded. A radiopaque ruler for measurement calibration was placed next to the coat during fluoroscopy and conventional x-ray. This step was not required in CT, as the measurements on a CT unit are precise within the vendor’s software. The length and width of all damage were measured digitally, and the results were recorded. Due to the uneven width of the damaged area, the widest section was considered.
As there are no official rejection criteria, the Lambert & McKeon [16] and Stam & Pillay [17] models were used to determine whether PPE was suitable for use in clinical settings based on defect size.
2.3. DosimetryIn the second part of the study, the transmittance of primary radiation through the protective layer was measured. Measurements were taken under both damaged and undamaged areas of the coats. In five damaged coats, the damage was too close to the border for the results to be representative, so they were excluded. Additionally, four coats exhibited the same type of material displacement, so only one of these was assessed. Measurements were conducted on eight damaged coats, two of which had two defects each, resulting in a total of twenty measurements (ten for damaged and ten for undamaged areas).
Transmission of the primary beam was measured using a GE Definium Tempo PRO x-ray device at 100 kV and 32 mAs, with a source-to-image distance of 100 cm. Each coat was closed as it would be when worn and positioned on the examination table with its anterior part facing the tube. A Raysafe X2 dosimeter (RaySafe, Sweden) was used for the measurements, with the X2 R/F sensor placed underneath the protective layer at both damaged and undamaged areas (0.35 mm Pb for one-piece and 0.50 mm Pb for two-piece coats).
Each measurement was repeated three times, and the average value was considered for further analysis. The following addapted equation, proposed by Zuguchi et al [19], was used to calculate the transmission ratio between damaged and undamaged areas:
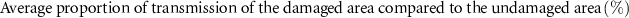
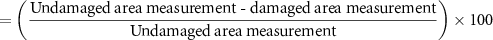 2.4. Statistical analysis
2.4. Statistical analysisResults were analysed using IBM SPSS Statistics 26.0 software (IBM, USA). Specificity, sensitivity, and accuracy were calculated to identify the most suitable test for detecting damage. According to the results of the study conducted by Chiegwu et al [20], damage was detected in 22.2% of all examined coats using visual-palpatory inspection. However, when the coats were examined with an x-ray source, damage was detected in 55.6% of all coats. Therefore, the x-ray method was considered the most reliable and proposed as the gold standard. Sensitivity, specificity, and accuracy were then calculated for the other methods. The Shapiro-Wilk test was used to assess the normality of the sample distribution. Because the data were non-normally distributed, a non-parametric Wilcoxon signed-rank test was performed to assess the impact of damaged PPE on radiation exposure. The Spearman correlation coefficient was calculated to assess the relationship between defect onset of defects and the age of the coats. A significance level of 5% was applied to all tests.
A total of 64 lead protective coats, all less than 15 years old according to the manufacturers, were included in the study: 50 two-piece coats with 0.5 mm Pb and 14 one-piece coats with 0.35 mm Pb.
3.1. Damage and the reliability of the examination methodsIn the first part of the study, damage was identified in 16 coats: 2 one-piece and 14 two-piece. Three of these coats had two defects each, resulting in a total of 19 detected defects. The proportion of damaged coats among those purchased in 2010, 2014, 2016, 2017, and 2019 was 100%, 54%, 21%, 17%, and 10% respectively, while no damage was observed in coats purchased in 2022. Based on the results of the Spearman correlation coefficient, a moderate correlation (0.523, p < 0.001) was observed between the age of the equipment and the onset of defects. Four different damage detection methods were used: visual-palpatory exam, light source examination, followed by x-ray-based examination with CT and fluoroscopy. All defects (n = 19) were visible on conventional x-ray and fluoroscopy; 94.7% (n = 18) were detected by CT, 73.6% (n = 14) by visual-palpatory assessment, and 47.4% (n = 9) by light source.
Visual and palpatory assessment demonstrated a sensitivity of 0.56, a specificity of 0.96, and an overall accuracy of 0.86. Assessment using a light source showed a lower sensitivity of 0.36, while achieving perfect specificity (1.00) and an accuracy of 0.84. In contrast, assessment using a CT unit yielded the highest diagnostic performance, with a sensitivity of 0.94, perfect specificity 1.00, and an overall accuracy of 0.98.
The visual-palpatory examination took approximately three minutes per coat. Light-based and CT examinations took five minutes per coat each, while fluoroscopy/x-ray examination took 10 min per one-piece coat and 15 min per two-piece coat.
3.2. Size measurementsMost defects were found in the skirt area of the coats. The size of each defect was measured using software integrated into the x-ray and CT devices. The measurement results are presented in table 1.
Table 1. Size and area of damage.
Size of damage of PPEArea of damaged PPEUsed evaluation methodIdentification number1 mm × 1 mm1 mm2X-ray1385 mm × 4 mm1540 mm2CT3395 mm × 11 mm4345 mm2CT749 mm × 3 mm147 mm2CT10150 mm × 3 mm450 mm2CT11335 mm × 3 mm1005 mm2X-ray12255 mm × 4 mm1020 mm2CT1863 mm × 3 mm189 mm2CT19240 mm × 4 mm960 mm2CT29355 mm × 15 mm5325 mm2X-ray31200 mm × 4 mm800 mm2CT54130 mm × 4 mm520 mm2CT54240 mm × 3 mm720 mm2CT553.3. DosimetryIn the second part of the study, eight coats were included in the dosimetric evaluation: six with one defect each and two with two defects each (n = 8). In the coats with two defects the average value was considered for further analysis. All coats were assessed for the amount of primary and secondary radiation transmitted through the protective layer.
3.4. Primary beam measurementsTable 2 presents the descriptive statistics of the primary beam transmittance measurements for damaged and undamaged areas.
Table 2. Descriptive statistics of the primary beam transmittance.
nAverage (µGy)Std. dev (µGy)Median (µGy)min. (µGy)max. (µGy)Undamaged area of the PPE8179.3117.9118.9114.7386.9Damaged area of the PPE8271.2165.6161.6121.9495.3The results of the non-parametric Wilcoxon test for related samples showed statistically significant differences between the transmittance of damaged and undamaged areas of PPE (p = 0.005). The transmittance ratio between damaged and undamaged areas was calculated for the primary beam, and the results of these calculations are presented in table 3.
Table 3. Proportion of transmittance of the damaged part in the primary beam.
Coat numberAverage transmittance ratio between damaged and undamaged areas (%)10.5340.911146.01218.01911.631316.648194.55422.8This study examined the integrity of 64 lead-based protective coats, aiming to identify the most reliable method for detecting defects in the protective layer and to assess the impact of damaged equipment on occupational exposure among medical staff. The results showed that 16 out of 64 coats had some form of defect; thus, 25% of the coats used in daily practice at the hospital where the study was conducted were damaged. It was observed that the age of the equipment plays an important role in the occurrence of damage, as no coats purchased in 2022 were damaged, while all coats purchased in 2010 were damaged. The proportion of damaged coats increased substantially with equipment age. This was further confirmed by statistical analysis, which showed a moderate correlation between equipment age and the occurrence of damage. This is consistent with the report published by the IAEA [13], which states that chemical changes in polymers caused by various factors can, over time, weaken the structure of the polymer and cause breakage. All coats were labelled with identification numbers from 1 to 64 to ensure traceability. Once damage was identified, the size of each defect was measured. As there is no standardised rejection criterion, two models were used to assess the adequacy of personal protective equipment. Based on the Stam and Pillay [17] model which considers both the length and location of the defect, 10 coats would be deemed inadequate, corresponding to 15.6% of all examined PPE. According to the Lambert and McKeon [16] assessment model, the size of the damaged area over overlapped, stitched, and posterior areas of the coat should not exceed 670 mm2. Based on this criterion, 12 out of 16 damaged coats would be eliminated, representing 18.8% of all examined PPE. In our study, the area of damage ranged from 1 mm2 to 5325 mm2, with an average damage size of 1309.4 mm2. When assessing the adequacy of PPE, it is important to consider not only the size but also the location of the defect. If the defect is located over a critical organ, reproductive organs, or the thyroid, the size limit for rejection is much lower (15 mm2 and 11 mm2 respectively) due to the greater radiosensitivity of these tissues [16, 17]. Defects located along seams, overlaps, or peripheral skirt regions generally have much higher clinical tolerances because these areas do not directly shield critical organs and often benefit from redundant layering. In contrast, even small defects situated directly over highly radiosensitive tissues can compromise protection to an unacceptable degree. This anatomical weighting is fundamental to the correct application of both the Stam and Pillay [17] and the Lambert and McKeon [16] models, ensuring that PPE assessment reflects not only the physical characteristics of the defect but also its clinical significance.
According to the DIN 6857–2 standard [15], seams, shoulder, waist, hip, central front areas, and overlap zones in wrap-around aprons are critical areas for damage development. A similar pattern was observed in our study, where the majority of defects appeared on the skirt area of coats, likely due to material folding from sitting, bending, or incorrect storage [6]. In five coats, defects appeared along the seams. A study by Kellens et al [6] reported that 34% of all damaged PPE exceeded the rejection criteria.
Four examination methods (visual-palpatory exam, light source inspection, CT and x-ray)were used as proposed by the DIN 6857–2 standard [15]. Results showed that examination with an LED light source is the least reliable method, as it detected only 47.4% (n = 9) of all damage. However, this method proved to be the most time-efficient, with assessment taking approximately 3 min per coat. Visual-palpatory exam, and CT assessments each took approximately 5 min per coat. Visual-palpatory examinations detected 73.6% (n = 14) of damage, while 94.7% (n = 18) of defects were detected by CT. This leads to the conclusion that the most reliable methods for detecting PPE damage are x-ray-based assessments using general fluoroscopy or a conventional x-ray unit, which detected 100% of all defects, followed by CT examination, which failed to detect only the smallest defect (1 mm2) that was visible only on fluoroscopy and conventional x-ray. This is also supported by the results of the statistical calculations of test accuracy, which were 0.98 for CT, 0.86 for visual-palpatory examination, and 0.84 for light source inspection. In terms of specificity, it was expected that x-ray assessment would confirm defects observed with other methods; however, estimated wrinkling in the protective layer was ruled out by x-ray-based assessment in two coats, resulting in a specificity value of 0.96. It is presumed that the undetected damage in the CT evaluation was due to exposing materials with high atomic numbers, such as lead, to a 120 kV imaging protocol, which produces pronounced metal artefacts, mainly from photon starvation. The extreme density contrast also amplifies partial volume averaging, causing severe distortion of the reconstructed signal. As a result, even small discontinuities within or adjacent to the material can be completely obscured. Under these conditions, a 1 mm air gap may be entirely masked in the final image. Based on this, the most cost-effective method would be CT evaluation, while the most precise method for damage evaluation of PPE would be x-ray or fluoroscopy.
Similar studies [14, 20] were conducted using slightly different methodological approaches. In 2016, the authors [14] detected damage in approximately 26% of all examined coats using CT imaging, while no damage were detected with visual or palpatory inspection. Chiegwu et al [20] reported that x-ray detected damage in 55.6% of all coats, while only 22.2% of all examined coats were reported as damaged using visual and palpatory inspection. Based on this, it can be concluded that x-ray-based assessment (conventional or fluoroscopy) remains an indispensable method for detecting damage in PPE. However, some concerns remain. Even though the DIN 6857–2 [15] standard calls for the use of remotely operated fluoroscopy devices, such devices may not be available everywhere, resulting in increased radiation exposure for the person performing the test and raising radiation protection concerns. X-ray assessment was also the most time-consuming, taking 10–15 min per coat. From this perspective, fluoroscopy would be the best method; however, if no remotely operated devices are available, such assessment can significantly increase radiation exposure for the person performing the assessment. Although it was proposed that x-ray detected all damage, this cannot be fully confirmed, as the coats would need to be taken apart and examined to determine whether any defect in the protective layer was missed.
In the second part of the study, the effect of damage to the protective layer on personnel exposure was investigated. Eight coats were included in the evaluation, two of which had two defects each. Other coats were excluded due to the close proximity of defects to the seams, which prevented accurate measurements, and because of the similarity in size and location of the damage; thus, only one coat was included in such cases, as results were expected to be similar. Transmittance of the primary beam through damaged and undamaged areas was measured. Statistically significant differences were found between damaged and undamaged areas (p = 0.005) in all assessed coats. The lowest average difference was observed in coat number 1, where transmittance through the damaged area was 0.5% greater compared to the undamaged area. The highest average difference was measured in coat number 31, where transmittance through the damaged area (355 mm × 15 mm) was 316.6% greater compared to the undamaged area. There was a major deviation in dose in one of the coats regardless of the imaging protocol. This was because the thickness of the lead equivalent in this coat was 0.35 mmPb, while in all others it was 0.5 mmPb. Similar findings were reported by Oyar and Kislaliglu [21] where transmittance was 7.1% at 0.35 mmPb and 3.9% at 0.5 mmPb. The difference in attenuation therefore appears even when no damage is present.
However, it must be emphasised that this dose is assumed only locally behind the damaged part of the PPE. From this it can be concluded that damage to the protective layer of the coat has an important impact on the dose, received by medical professionals. Although personnel are not exposed to the primary beam during imaging, some level of scattered radiation can penetrate the damaged area, leading to increased radiation exposure. Although the doses received from damage to the protective layer are usually not high enough to cause significant deterministic effects, the risk of stochastic effects remains, as no level of radiation is considered safe and even small doses can increase the likelihood of developing cancer over a lifetime [22]. Therefore, it is important to conduct regular testing of PPE to ensure its adequacy and thereby contribute to the safety of employees.
Although the study showed clear results, certain limitations remain: x-ray imaging was chosen as the gold standard, but it cannot be claimed that it detected all defects, as the coats were not disassembled and the protective layer was not examined for missed or microscopic damage. The area of the damage was only an approximation and was not calculated in detail, as only the widest part of the defect was considered.
During the study, damage was observed in 25% of all tested protective coats. Of all assessed coats, 15.6%–18.8% were deemed inadequate and should be eliminated according to the Stam & Pillay or Lambert & McKeon rejection models, respectively. Among the four examination methods proposed by the DIN standard, x-ray-based assessment using fluoroscopy/x-ray was the most reliable for detecting damage (100%), followed by CT (94.7%). While x-ray-based evaluation is more precise, CT-based evaluation is the most time- and cost-effective method, although it can miss some small defects in the PPE. Transmittance of primary radiation in all coats was significantly higher through damaged areas for all protocols (p = 0.005). Based on the dosimetric reports and comparisons between damaged and undamaged areas, regular quality assessment of PPE is recommended to ensure an adequate level of radiation protection and safety, thereby minimizing potential harmful effects of radiation. Therefore, it is advisable to conduct annual PPE inspections and include them in the QC report, together with the annual QA and QC tests of the x-ray units performed by the medical physicist taking into account logistical feasibility of such testing.
The data cannot be made publicly available upon publication because they are owned by a third party and the terms of use prevent public distribution. The data that support the findings of this study are available upon reasonable request from the authors. To ensure appropriate use and interpretation of the data, the datasets are not publicly available.
Comments (0)