Telemedicine integration across various specialties has surged globally, bridging healthcare gaps by reducing logistics, cutting costs, and enabling timely care.1 Paediatric dermatology, often reliant on urban-based specialists with limited rural access, differs from adult dermatology in disease prevalence, presentation, and the need for specialised knowledge. Barriers to dermatology are pronounced in children due to subtler symptoms, varied morphology, and reliance on parental support.2–5 Access is further constrained in underserved communities by geographic, financial, language, and cultural barriers; making paediatric teledermatology (PTD) a promising solution.6–10
This six-month analytical cross-sectional study explores factors that optimise PTD care in resource-limited settings using e-Sanjeevani 2.0 platform— a public health telemedicine initiative by the Government of India, operating on a ‘hub-and-spoke’ model, connecting referring healthcare providers (RHPs) at peripheral centres to specialists at higher centres for real-time, secure ‘provider-to-provider’ interactions through audiovisuals, images, and texts11,12 [Figure 1]. Integrating basic examinations performed by RHPs with detailed assessments by specialists, including the generation of e-prescriptions, e-Sanjeevani is the largest documented telemedicine initiative in primary healthcare worldwide.13,14 This study, conducted at a tertiary centre ‘hub’ for cases from Haryana, examines the scope, feasibility, utilisation, clinico-demographics, operational aspects, and provider perceptions of delivering dermatological care to children via telemedicine.
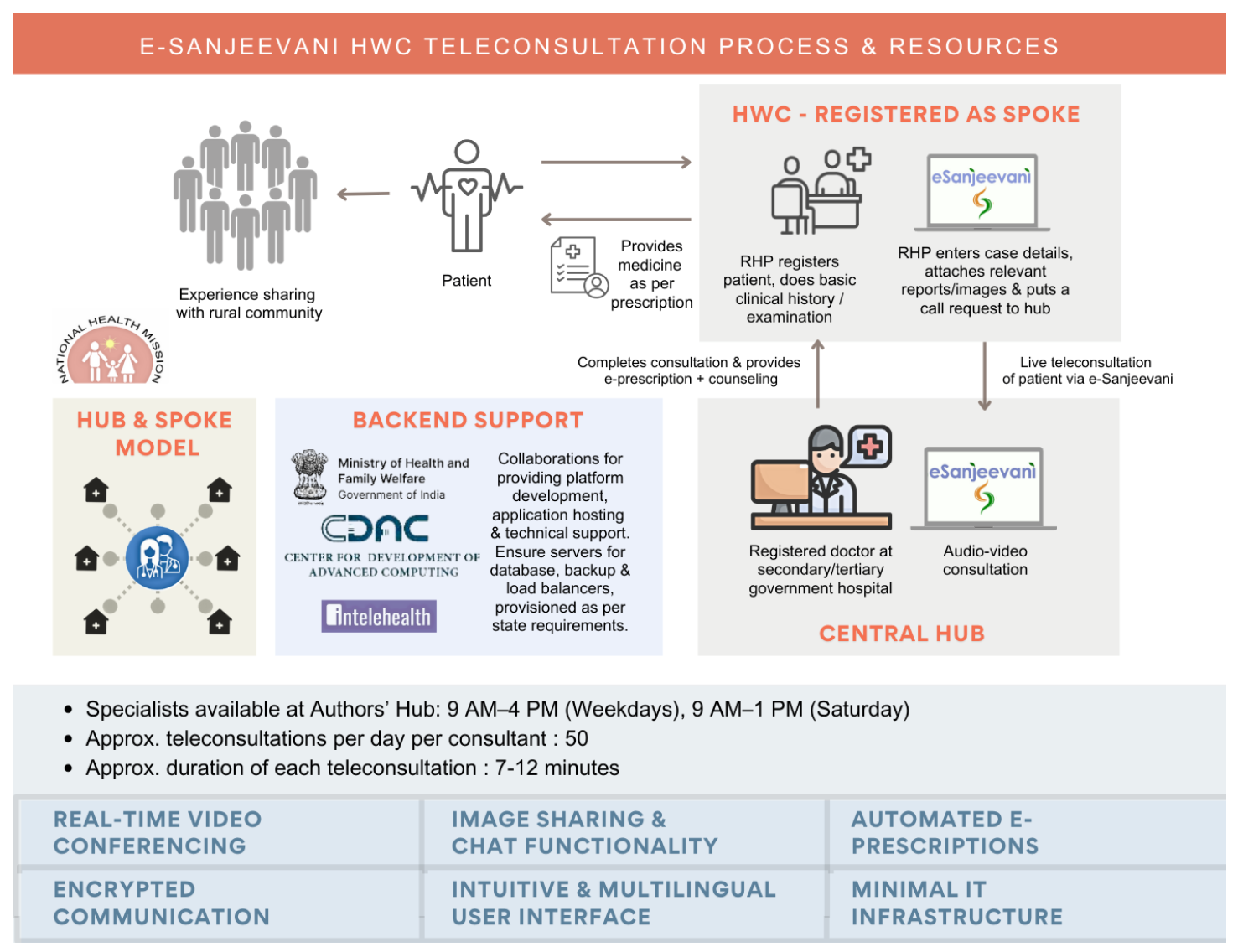
Export to PPT
MethodsStudy design & Population: Data were gathered cross-sectionally from individual PTD consultations, complemented by a retrospective survey capturing RHPs’ overall experiences and perceptions. Participants ranged from neonates to 18-year-olds, seeking remote consultations for dermatological conditions, recruited via consecutive sampling at the authors’ tertiary centre over six months (August 2023 to January 2024). Cases lacking clear photographs or provisional diagnoses were excluded. The study received ethical approval and adhered to the Declaration of Helsinki. Informed verbal consent was obtained from the parents/guardians before teleconsultations, as required by national telemedicine guidelines for consultations initiated by RHPs. The e-Sanjeevani 2.0 platform complies with relevant data protection regulations, and all data were anonymised.11,12
Data collection & Variables: Standardised data collection forms captured demographic details, consultation specifics, and provider perceptions. Consultation data were compiled by technical support into Excel sheets. Four consultation variables were assessed for their impact on physician confidence in diagnosis and management: image quality, multiple images, audiovisual/text interaction, and ancillary (past/medical/family) patient history. Acute/emergency cases managed empirically and those requiring referral were assessed. RHPs’ perspectives were evaluated via a retrospective Google form survey, assessing comfort with the service, educational benefits, and perceived parental/guardian satisfaction (1-5 scale) [Supplemental-data].
Statistical analysis: Analyses were performed using SPSS v22 (IBM Corp., Armonk, NY). Descriptive statistics were used to summarise the data. Friedman test assessed differences in perceived helpfulness, and pairwise comparisons were made using the Wilcoxon Signed Ranks test, considering p<0.05 as significant and p<0.001 highly significant.
ResultsDemographics and clinical characteristics: The study included 961 children (median age: 5 years, IQR: 2–11; 52.1% female). Most diagnoses were infections and infestations, followed by dermatitis, while naevi and tumours were least common [Figure 2]. The follow-up rate for teleconsultations on the platform was 9.6%. Only 43 cases (4.47%) required in-person consultations for acute dermatoses, including 13 emergency/acute cases (1.35%), empirically managed per national telemedicine guidelines along with urgent referral for in-person care12 [Table 1].
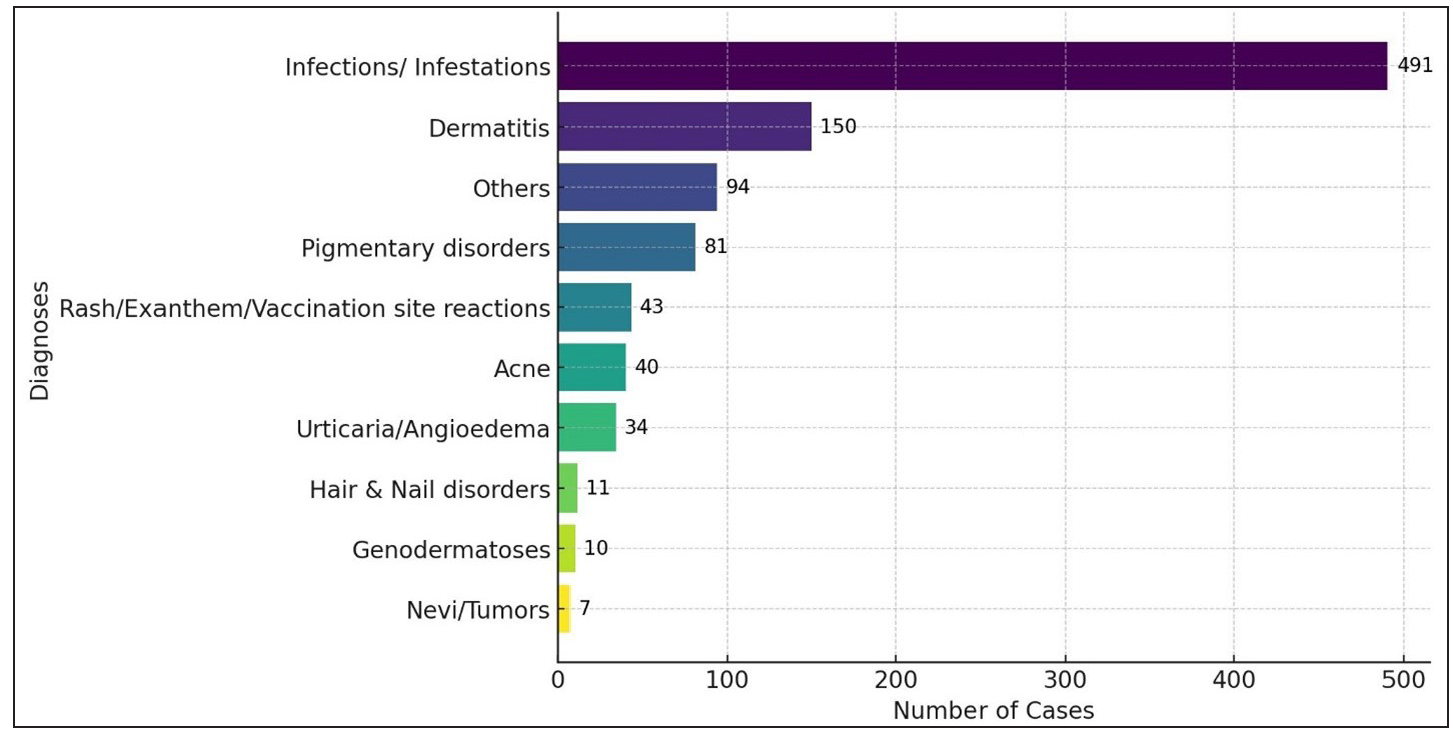
Export to PPT
Table 1: Table illustrating the distribution and characteristics of emergency/acute and referred paediatric tele-dermatology cases in the study.
Category Cases (%) Examples Emergency/Acute Dermatoses managed empirically 13 (1.35) Angioedema, burns, Stevens-Johnson syndrome, omphalitis, neonatal candidiasis, staphylococcal scalded skin syndrome, acne fulminans Referrals for in-person care 43 (4.47)Acute Dermatoses: Same as above.
Procedures: Warts, molluscum contagiosum, pyogenic granuloma, keloids/scars.
Biopsy/Further evaluation: Mycetoma, scrofuloderma.
Complex cases requiring in-person care: Ulcerated haemangiomas, rapidly progressive vitiligo, psychodermatoses (e.g., dermatitis artefacta, trichotillomania), concomitant malnutrition in acrodermatitis enteropathica, genodermatoses (e.g., epidermolysis bullosa, Peutz-Jeghers syndrome)
Consultation characteristics: The helpfulness of consultation variables for PTD case management was rated on a three-point scale: (1)Not helpful—diagnosis and treatment were confidently made without it; (2)Somewhat helpful—contributory but not essential; (3)Very helpful—critical for diagnosis or treatment. Image quality was ‘very helpful’ in 79.1% of cases, followed by audiovisual/text interactions (50.1% rated ‘very helpful’). Multiple images were rated ‘somewhat helpful’ in 40.5% of cases, while ‘ancillary’ (past/medical/family) history was deemed ‘not helpful’ in 65.1% of cases [Table 2; Figures 3a,3b]. A Friedman test revealed significant differences in perceived helpfulness across the four consultation variables (χ2 (3, N=961) =1463.075, p<0.001). Wilcoxon Signed Ranks tests showed highly significant differences between each pair (p<0.001), with Image Quality being the most helpful, followed by Audiovisual/Text Interaction, Multiple Images, and Past/Medical/Family History [Table 3]. Although multiple images were rated as ‘somewhat helpful’ and ancillary history as ‘not helpful’ overall, they were particularly considered ‘very helpful’ for diagnoses like rashes, acne, vitiligo (multiple images), scabies and impetigo (ancillary history).
Table 2: Table summarising descriptive statistics of how helpful each consultation variable was in diagnosing/managing paediatric dermatological cases through eSanjeevani 2.0.
Consultation VariableHelpfulness ratings
1 = not helpful (minimum)
2 = somewhat helpful
3 = very helpful (maximum)
Helpfulness ratings
Number of cases (% of cases)
Mean rating ± SD Median rating (range 1 to 3) Not helpful Somewhat helpful Very helpful Total cases Quality of image 2.78 ± 0.442 3 11 (1.1%) 190 (19.8%) 760 (79.1%) 961 (100%) Multiple images 1.85 ± 0.757 2 358 (37.2%) 389 (40.5%) 214 (22.3%) 961 (100%) Audiovisual/text interaction 2.43 ± 0.625 3 70 (7.3%) 410 (42.6%) 481 (50.1%) 961 (100%) Past/ medical/ family history 1.46 ± 0.685 1 626 (65.2%) 229 (23.8%) 106 (11%) 961 (100%)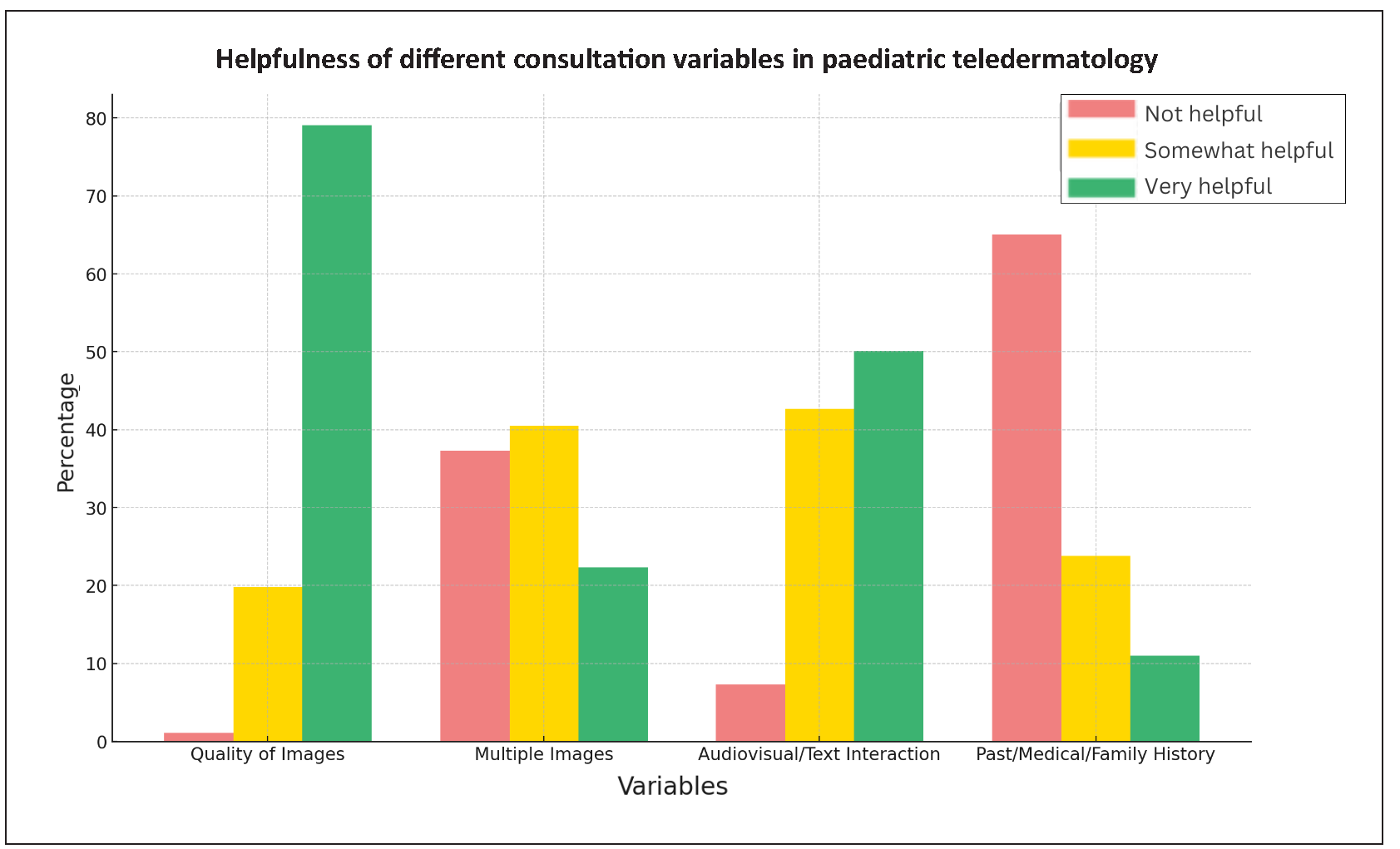
Export to PPT

Export to PPT
Table 3: Wilcoxon Signed Ranks test results for pairwise comparison between consultation variables. *
Comparison Z value p-value More helpful variable Quality of images vs. Multiple images 22.846 < .001 Quality of images Quality of images vs. Audiovisual/Text interaction 13.156 < .001 Quality of images Quality of images vs. Past/medical/family History 24.859 < .001 Quality of images Audiovisual/Text Interaction vs. Multiple Images 15.909 < .001 Audiovisual/Text interaction Multiple Images vs. Past/Medical/Family History 11.602 < .001 Multiple images Audiovisual/Text Interaction vs. Past/Medical/Family history 22.984 < .001 Audiovisual/Text interactionRHP perception: Links to the online (Google Form) survey were sent to the 185 RHPs who had consulted the hub for PTD cases over six months, of which 107 responded (57.83% response rate). RHPs viewed the service positively, noting substantial clinical and educational value [Table 4]. The high mean satisfaction rating (4.47 on a 1-5 scale) with a low standard deviation (0.87) demonstrated consistent satisfaction among parents/guardians, as reported by RHPs. Chi-square tests showed no significant differences in comfort, outcomes perception, recommendations, or satisfaction across different RHPs and centre types, suggesting uniformly positive perceptions of PTD. Centre types follow India’s primary healthcare hierarchy by population size, ensuring equitable care [Figure 4].
Table 4: Receptivity and effectiveness of paediatric tele-dermatology consultations on the eSanjeevani 2.0 platform, based on the RHP survey.
Parameter Result Inference Comfort with platform 100% Comfortable All providers were comfortable using the telemedicine platform for PTD cases. Parent/Guardian satisfaction Mean: 4.47 (on a scale of 1-5), SD: 0.87 High and consistent satisfaction levels among parents/guardians. Perception of treatment outcomes amongst RHPs 84.11% believe online is almost as good as in-person. Majority were confident in PTD, some preferred in-person consultations. Educational benefits of service 98.13% enabled better management. Nearly all providers feel better prepared to manage future cases.Recommendation of
e-Sanjeevani for paediatric cases
with skin concerns
96.26% Would recommend, 3.74% Would not Strong endorsement of the platform by providers.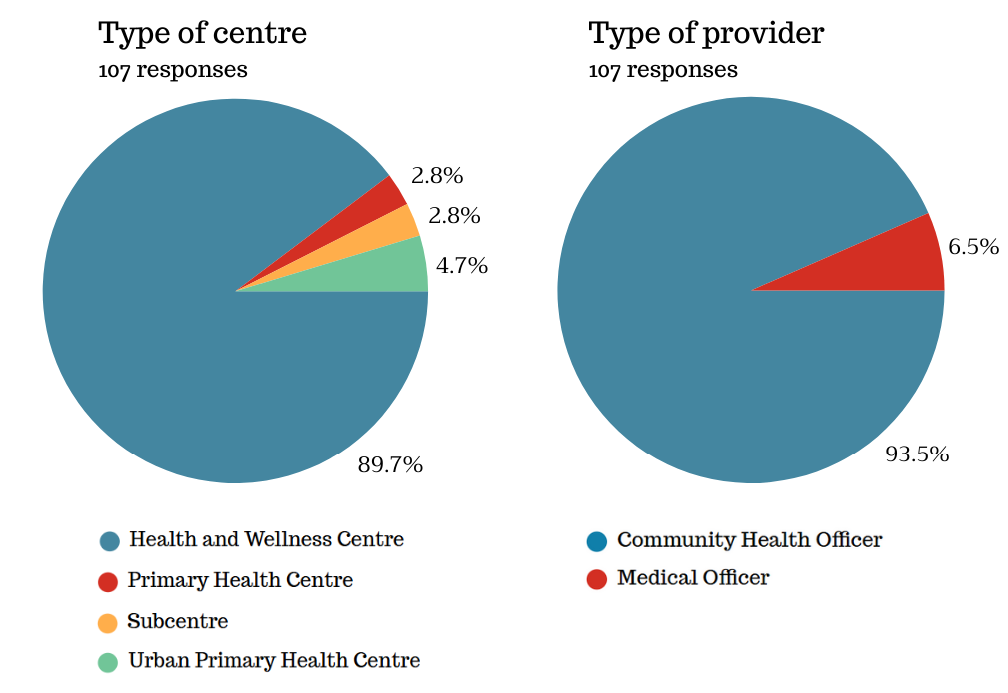
Export to PPT
DiscussionThe existing literature on PTD mostly from Western sources and focussed on store-and-forward (asynchronous) systems. In contrast, this study offers key insights into PTD in a developing country, using a well-established telemedicine platform to address a wide spectrum of dermatological disorders in a large paediatric cohort from underserved communities.
Quality of image was significantly more helpful than other consultation variables for diagnosing and tailoring management. While studies have shown mixed results regarding image quality’s impact on diagnosis alone, most emphasise its importance.5,15-18 The next key factor was audio-video communication, suggesting that real-time (synchronous) teledermatology systems may be more effective than asynchronous ones, though further validation is needed. Ancillary patient history, while valuable in traditional clinical settings, was relatively less useful in PTD where audiovisual assessment predominates. Hence, PTD systems should prioritise good audio-video connectivity and training providers to capture high-quality, representative images over extensive historical data collection.15
While certain variables were less helpful, their value should not be undermined. Multiple images, though mostly ‘somewhat helpful,’ proved valuable for dermatoses requiring assessment of extent/distribution/severity to guide management, and those with varied clinical morphologies, including rashes (atopic dermatitis, seborrheic dermatitis, chickenpox), acne, and vitiligo. This aligns with Philips et al.’s findings on the importance of multiple images for childhood rashes.16 Ancillary history, though of limited overall utility, was ‘very helpful’ in 11% of cases, especially contagious dermatoses like scabies and impetigo, where understanding family contacts and living conditions aided management. Infections and infestations were the most common diagnoses in this cohort, while naevi and tumours were least common, contrasting with Western PTD studies that report more naevi.10,19
Emergency/acute dermatoses, comprising 1.35% of PTD cases, were advised for immediate in-person interaction as per national telemedicine guidelines. Teleconsultations facilitated necessary immediate interventions such as appropriately-dosed empirical antibiotics/antivirals/steroids, monitoring, counselling on local care, and urgent referral to higher centres. Overall, only a small percentage (4.47%) of cases required referrals for in-person evaluation, including these emergency/acute cases [Table 1]. This suggests that a majority (95.53%) of first-time, low-complexity, non-procedural cases could be managed remotely, demonstrating PTD’s utility in situations where immediate in-person specialist care is unavailable. The process also serves as an effective triage system, determining the necessity and urgency of referrals and preventing complications.3,10,12 RHPs strongly endorsed the service, rating it nearly as effective as in-person care for PTD, with added educational benefits, aligning with previous reports demonstrating bidirectional learning.15,17,20 Another assisted telemedicine model, ‘e-consults’ in the US, which uses the store-and-forward format, showed comparable provider satisfaction.15,17 Parental/guardian satisfaction ratings likely reflect growing acceptance due to convenience, live specialist interactions, reduced wait times, cost savings, accessibility, and avoiding the logistical challenges of traveling with young children or missing work/school.1,3,10,15,21 Previous studies report higher parental satisfaction with synchronous (real-time) PTD compared to store-and-forward systems, though comparative trials are lacking.1,15,21 While diagnostic and management concordance could not be assessed, prior studies report concordance rates of 70.1%-89%.1,15,16,22-25
LimitationsThe study had several limitations. Diagnostic and management concordance could not be assessed, as referred cases were not always evaluated at the authors’ centre, precluding direct comparisons between telemedicine and in-person diagnoses. The diagnostic discordance in this study remains unclear, warranting further investigation. The telemedicine model resulted in an average travel distance saved of 459 km per patient, likely influencing decisions regarding in-person consultations. The 9.6% follow-up rate, reflecting only platform re-consultations, was lower than that in studies with shorter travel distances or in-person follow-ups. Other limitations included short duration, potentially missing seasonal variations in paediatric dermatoses, and restriction of the study population to those able to access peripheral ‘spoke’ centres, despite minimised selection bias through consecutive sampling. Additionally, patient-reported outcomes and operational factors like connectivity, video quality, and cost-effectiveness were not assessed. Future multi-centre studies should address these gaps, particularly in evaluating diagnostic accuracy through direct comparisons with in-person evaluations.
ConclusionThis study demonstrates the feasibility and effectiveness of PTD in marginalised areas in a developing country, highlighting its utility to manage routine cases, empirically treat emergency dermatoses, and serve as a triage tool. The integration of e-Sanjeevani into India’s healthcare infrastructure offers a functional foundation for further upscaling PTD services. Enhancements should focus on optimising image quality, enabling audiovisual communication, refining historical data usage, and continuing training for RHPs. It is hoped that the insights gained will help bridge gaps in paediatric dermatological care, particularly in remote resource-constrained settings.
Comments (0)